Chantal Edge is a Specialty Registrar in Public Health and an NIHR Clinical Doctoral Research Fellow, researching prison video consultations (telemedicine). She has been assisting NHS England and NHS Improvement with the national rollout of telemedicine across secure settings as part of the pandemic response. She recently delivered a webinar in partnership with Clinks on telemedicine in secure settings and how the voluntary sector can use it.
When the Covid-19 pandemic hit in early 2020, community-based health care services in England were quick to react, and swiftly adopted video consultations as a means to deliver health care remotely. Patients quickly accepted that if they needed to see their doctor, they might do it over MS Teams or Zoom, and a whole range of new video consultation platforms sprung up overnight to assist with delivering these appointments.
What was happening in secure environments such as prisons, immigration removal centres and the children’s secure estate? Traditionally, it’s always been quite hard to introduce new technologies into these settings. Her Majesty’s Prison and Probation Service (HMPPS) has to centrally approve any technology that goes into its sites, to assure safety and security around the proposed systems. However, with the threat posed to healthcare continuity by Covid-19, the HMPPS digital teams offered immediate support to NHS England and NHS Improvement to rapidly approve technology for video consultations (also called telemedicine) in secure settings. This even included changing national policy in just four days to allow use of 4G tablets for video consultations, which prior to this legislation change would have been considered illegal.
As a result, all prisons, immigration removal centres and children’s establishments in England now have the capability to make video calls for health related services. These sites can undertake video calls on both the PCs in healthcare and on their 4G tablets to connect patients to clinicians or services based outside of their secure site. The system has been configured so that it meets HMPPS rules (for example, it provides a clear audit trail of calls) but is also suitable for healthcare needs. As expected, there are some rules around how video consultations can be used which can be seen in the figure below:
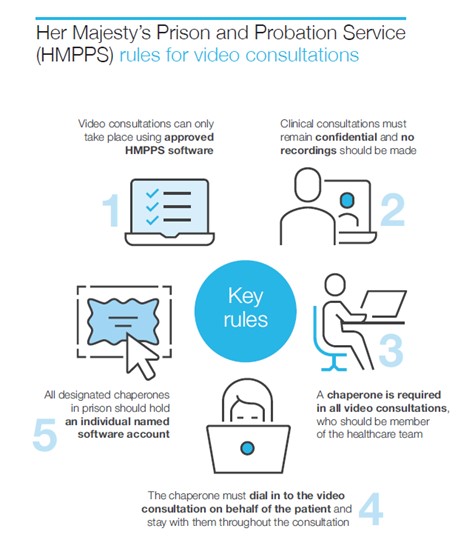
How can secure sites use video consultations?
The video consultation system has been set up so that secure sites can dial each other (e.g. prison to prison), as well as services outside of the justice system. This could include general hospitals, GPs working at home, forensic hospitals, or of course voluntary sector providers. Some examples of the types of calls secure sites might want to make are shown in the figure below, however this list is by no means exhaustive.

The purpose of setting up this video consultation service is two-fold. Firstly, to make sure people in the criminal justice system get the same opportunity to access healthcare remotely as the community throughout the pandemic. At the first peak of the pandemic a huge proportion of health care contact was taking place online. By failing to offer an equivalent option, people in secure settings could be really disadvantaged in future waves of Covid-19, which would only serve to exacerbate health inequalities experienced by people in contact with the criminal justice system. Secondly, the world in general is moving towards a new digital wave of health care delivery, which was accelerated by the pandemic situation. Video consultations are likely here to stay in some format. Having the option for remote service delivery in prisons is both equivalent to what is available in the community, but also opens doors to better access to a wider range of services and hopefully offers a better experience than going off-site to hospitals in handcuffs.
Why is this relevant to the voluntary sector?
I recently did a webinar with Clinks to try and get the word out to voluntary sector services that the telemedicine service now exists in secure settings, and the opportunity to consider whether their health related services might be able to make use of video consultations in some way. We asked people where they thought video consultations could potentially be used in secure settings for voluntary sector services, suggestions included:
- Housing assessments
- Psychosocial support
- Improved patient outcomes
- Substance misuse services
- Preparation for rehab
- Through the gate prep
- Remote key-working
- Antenatal groups
- Counselling
Following on from this we’d like more of the voluntary sector services to consider:
Do you think your organisation could make use of the video consultation model in secure settings for service delivery?
What do you think your organisation could use video consultations for?
Is this useful purely for pandemic service continuity, or do you think it could become a useful model outside of pandemic situations?
Next steps
If you think there might be a role for video consultations in your service, the first step is speak to your local prison/ immigration removal centre/ children’s secure estate healthcare team or health and justice commissioner. The secure setting healthcare team will probably have to send you an online meeting link for appointments, and they will need to provide a chaperone to sit in the consultation, so it’s really crucial to talk to them early to see how this could work. If you don’t know the contacts at your local secure settings then NHS England can help – every site has a telemedicine champion from the healthcare team. If you want to be put in touch with your local champion, please email england.healthandjustice@nhs.net stating which establishments you are interested in working with and what type of services you are interested in providing by video. You are also welcome to join the NHS Futures Collaboration platform for secure setting telemedicine.
Moving forward, we will be evaluating the telemedicine service over the next few years. NHS England and NHS Improvement have funded the telemedicine service for a two year pilot period (2020-2022), so it’s also really important that we gather information to understand whether it is worth re-investing in this service at the end of this pilot.
But most importantly, we will want to understand how patients experience it, and whether it improves the access and quality of the services they receive, both during and beyond Covid-19.
Cover photo: Nilaari | © Ian Cuthbert cuthbertdesign.com
What's new
Blogs
Senedd Elections – A Sector Briefing
Publications
Clinks Families Network - Memorandum of Understanding (MoU)
This Memorandum of Understanding sets
Latest on X
The role is for a leader from an organisation focused on racially minoritised people, with expertise in service delivery, policy, advocacy, or related areas in criminal justice. Racial disparities are present at every CJS stage. This role ensures these voices are central in shaping policy to help address and eradicate them. Apply by Mon 18 Nov, 10am. More info: https://www.clinks.org/voluntary-community-sector/vacancies/15566 #CriminalJustice #RR3 #RacialEquity

